HoverTech News
Educational content, new product announcements, business articles, and more.

Navigating Phantom Pain and Vascular Post‑Operative Ambulation
Vascular surgery patients have an elevated risk of falls and diminished health outcomes – risks heightened by ambulation barriers that sometimes include phantom limb pain. Discover tips for safely and efficiently ambulating post-operative vascular patients, including amputation patients. Listen to the full on-demand webinar to earn one contact hour. Vascular surgery patients – those undergoing open or minimally invasive blood flow-related procedures [...] Read More

You Have an SPHM Policy – But Can Staff Follow It? Lessons Learned from Medical Malpractice Lawsuits
Medical malpractice lawsuits are on the rise. They can shed light on safe patient handling and mobility (SPHM) practice and policy weaknesses – weaknesses capable of putting nursing licenses and entire organizations on the line and even on the stand. Discover tips for assessing and improving your SPHM protocols and procedures and listen to the full on-demand webinar to earn [...] Read More
Stay Up-to-Date on Everything Hovertech
Sign up for our newsletter and receive regular updates and important healthcare news from the company

Becoming a Stronger Nurse Leader
Ready to sharpen your workplace leadership skills? Read on for time-proven nursing career tips – including the one trait considered non-negotiable among effective nurses. Listen to the full on-demand webinar to earn one contact hour. It can be hard to pinpoint... Read More

Practical Tips for Diversity, Equity, and Inclusion in Bariatric Patient Population SPHM and Care
A growing bariatric patient population warrants new approaches to DEI initiatives in SPHM – philosophically, but also practically. Read on for helpful guidelines and listen to the full on-demand webinar to earn one contact hour. Obesity rates continue to climb... Read More
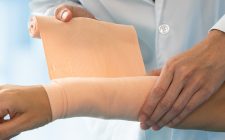
Minimizing Pain, Maximizing Movement: SPHM for Severe Burn Patients
Listen to the Supplementary, Free Webinar on Moving Patients with Severe Burns Nursing intervention for burns presents unique and high-stakes challenges. Read on for helpful guidelines and listen to the full on-demand webinar to earn one contact hour. Please note:... Read More

ICU Pressure Injuries: Unique Risk Factors and Skin Assessment Tips
Listen to the Supplementary, Free Webinar on ICU Pressure Injuries Pressure injuries in critical care settings are common, clinically catastrophic, and costly. Read on for helpful prevention guidelines and listen to our on-demand webinar to earn one contact hour. When acute... Read More

HoverCover™ Disposable Absorbent Cover Promotes Skin Integrity
Tampa General Hospital is one of Florida’s largest hospitals, ranked top in the state for 2022-23 by U.S. News and World Report. Earlier this year, they admitted a patient weighing more than 750 pounds. Because of various conditions requiring extended... Read More

4 Steps to Truly Effective Safe Patient Handling and Mobility (SPHM)
Earn one contact hour. Listen to the supplementary, free webinar on SPHM competency. Dusting off your acute care setting’s SPHM practices is key to fewer injuries and stronger outcomes. Read on for helpful guidelines + listen to our on-demand webinar... Read More

Laparoscopic Cholecystectomies: Pre‑Operative Considerations for New Nurses
Earn one contact hour. Listen to the full, free webinar on pre-operative considerations for laparoscopic cholecystectomies. This seemingly routine surgical procedure is actually quite complex. Listen to our full webinar recording on the topic to earn one contact hour. Read on... Read More
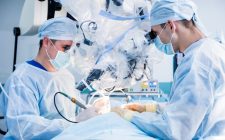
Keeping Patients and Staff Safe During Perioperative Spinal Surgery Prone Positioning
Download the FREE resource guide Download the FREE resource guide: Alternatives to Manual Prone Positioning PDF Listen to HoverTech’s webinar on Safe Patient Handling During Spinal Surgery and earn one contact hour! Spinal procedures are among the most commonly performed medical procedures... Read More

Preventing Patient Falls: 8 Overlooked Tips and Tools
Download the FREE tip guide We find that some of the most overlooked fall prevention tactics are also the simplest. Want to keep these tips handy? Download the 8 Tips & Tools For Preventing Patient Falls. Rapid Response Team – fall! As a... Read More

Critical Care Crib Sheet: 7 Tips from a Longtime ICU Nurse
We see you, ICU nurses – tackling high stakes shift after shift, often with too few resources. You’ve been essential frontline workers since before they were buzzwords, displaying unmatched resilience that can come at a cost: In a 2021 study... Read More

Less Support, Same Expectations: Nurses Working with Limited Resources
The nurse staffing crisis is no secret – and no laughing matter. An astounding 18% of nurses have resigned from jobs since 20201 , most citing burnout from COVID’s heightened risks and expectations. Many nurses who aren’t changing fields... Read More

Nobody Has to Get Hurt: Smarter Handling Solutions Protect Nurses, Caregivers, & Their Patients
The importance of patient repositioning is well known in healthcare. It’s also a Catch-22: The more often nurses and caregivers manually reposition bedridden patients, the more likely they are to incur injuries themselves. COVID made matters worse by increasing... Read More
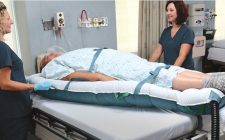
Reduction in Patient Handling Injuries by Promoting a Culture of Safety and Use of Air‑Assistive Technologies
After noticing a dramatic increase in patient handling related injuries to staff, the University of Rochester Medical Center’s (URMC) facility, Strong Medical Center, decided to investigate the cause. They found that many of their staff members didn’t use the... Read More

The Heavy Cost of Improper Lifting
HoverTech International’s product engineering – how they work – tends to take center stage in conversations, for good reason. The HoverMatt® Air Transfer Mattress, HoverSling® Transfer and Lift System, and HoverJack® Air Patient Lift are remarkably visual, with design... Read More

Safe Patient Handling and Mobility in Med‑Surg Nursing Webinar
ALLENTOWN, Pa., December 4, 2020 — Join us on December 17ᵗʰ at 3pm EST for our Safe Patient Handling and Mobility in Med-Surg Nursing webinar. We’re offering one (1) Contact Hour... Read More
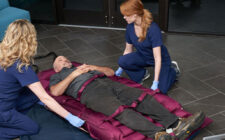
Safer Solutions for Fall Recovery in the Healthcare Setting
ALLENTOWN, Pa., June 28, 2019 — Each year, somewhere between 700,000 and 1,000,000 people in the United States fall in the hospital.1 With this prevalence of patient, staff and visitor falls, healthcare facilities require fall recovery solutions that are... Read More